Status: Individual prior approval
Effective date: 1 April 2026
Next review date: 1 April 2028
Essex ICB commissions interventional treatment for varicose veins on a restrictive basis.
For the purposes of this policy, “Grade III and above” corresponds to CEAP* clinical classes C3–C6, which include oedema (C3), skin changes such as venous eczema, pigmentation or lipodermatosclerosis (C4), healed venous ulceration (C5) and active venous ulceration (C6).
CEAP*- Clinical–Etiological–Anatomical–Pathophysiological, the internationally recognised classification system used to categorise the severity and features of chronic venous disease, including varicose veins.
Conservative management is the first line of treatment and applications will not normally be accepted without evidence that conservative management of asymptomatic and symptomatic varicose veins has been tried, and failed, for a period of at least six months.
Prior to consideration for intervention patients should be given information regarding:
- Weight loss if they have a raised BMI.
- Light to moderate physical activity
- Avoiding factors which are known to make their symptoms worse, if possible
- Use of compression stockings for a 6-month duration, where this is considered appropriate.
- When and where to seek further medical help
Interventional treatment is not routinely funded for CEAP C2 varicose veins, which are symptomatic but without complications.
Funding for treatment will only be approved for Grade III and above varicose veins (CEAP C3–C6). This includes patients with complications such as bleeding, recurrent thrombophlebitis, venous eczema, lipodermatosclerosis or venous ulceration.
Although NICE CG168 recommends referral for all symptomatic varicose veins, including CEAP C2 disease, Essex ICB commissions interventional treatment only for patients with complications (CEAP C3–C6). This divergence from NICE reflects local prioritisation of finite NHS resources towards those with the greatest clinical need.
Grade III: Varicose veins with complications, including bleeding, recurrent phlebitis or eczema.
- Patients who have had bleeding associated with varicose veins should be referred urgently.
- Patients with recurrent thrombophlebitis and persistent varicose veins may be referred, especially if phlebitis has affected veins above the knee.
- Patients with eczema near the ankle or associated with varicose veins below the knee should be referred for specialist advice.
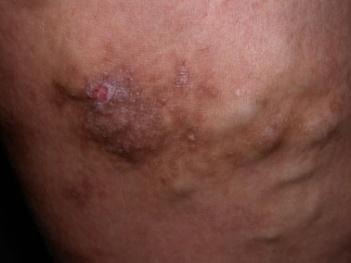
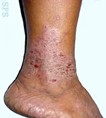
Varicose Eczema Stasis Gravitational Eczema
Interventional treatment should be in line with NICE guidance which identifies endothermal ablation as the first line intervention where suitable. If endothermal ablation is unsuitable, offer ultrasound-guided foam sclerotherapy. If ultrasound-guided foam sclerotherapy is unsuitable, offer surgery.
Do not carry out interventional treatment for varicose veins during pregnancy other than in exceptional circumstances. Consider compression hosiery for symptom relief of leg swelling associated with varicose veins during pregnancy.
Patients whose veins are purely cosmetic and are not associated with any symptoms will not be funded. Do not refer for NHS treatment.
Patients not meeting the above criteria will not be funded unless there are clinically exceptional circumstances.
Individual funding requests should only be made where the patient demonstrates clinical exceptionality.
Further information on applying for funding in exceptional clinical circumstances can be found on the ICB website.
References:
Varicose veins: diagnosis and management Clinical guideline [CG168] Published: 24 July 2013